U.S. Antibiotic Awareness Week: An Update on the Antimicrobial Use Option
U.S. Antibiotic Awareness Week (USAAW) raises awareness about appropriate antimicrobial use and the threat of antimicrobial resistance. More than 2.8 million antimicrobial-resistant infections occur in the United States each year, and more than 35,000 people die as a result.[1] Improving antimicrobial use improves the treatment of infections, protects patients from preventable harms from antimicrobials, and reduces antimicrobial resistance. Patients infected with antimicrobial-resistant organisms have longer, more expensive hospital stays and may be more likely to die because of their infection.[2]
Studies show providing timely and reliable information to clinicians regarding their prescribing practices, as part of a coordinated effort known as antimicrobial stewardship, can improve antimicrobial use.[3],[4],[5] Antimicrobial stewardship combats antimicrobial resistance, in part, by measuring and improving prescribing practices by clinicians.
The Centers for Disease Control and Prevention (CDC) launched the National Healthcare Safety Network (NHSN) Antimicrobial Use (AU) Option in 2011 to provide a mechanism for hospitals to report and analyze antimicrobial use. In honor of USAAW 2019 and Lantana’s continued partnership with the CDC, we put together an update on the NHSN AU Option.
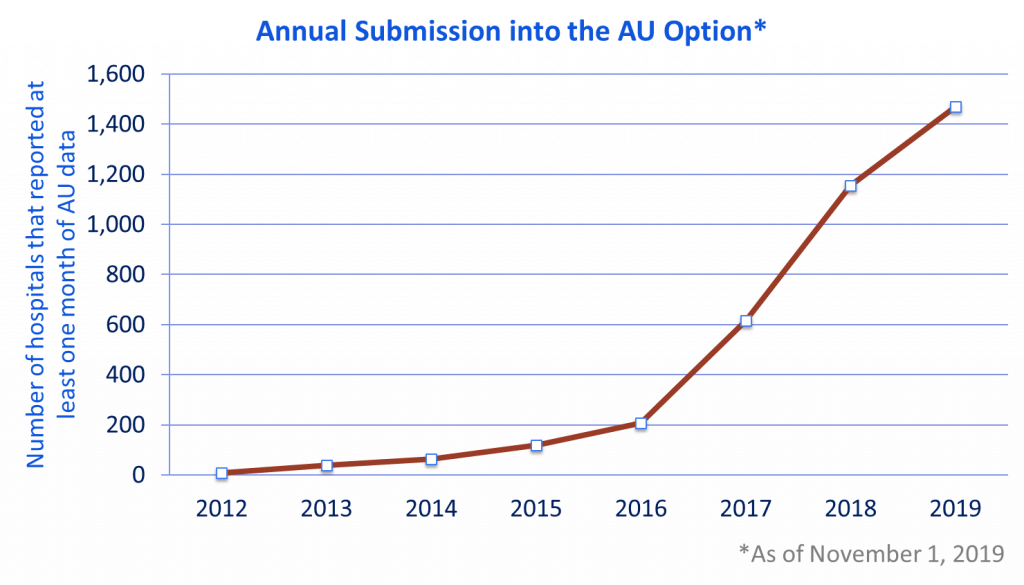
AU Option enrollment grew from just 40 hospitals at the end of 2013 to over 1,400 hospitals today through partner engagement and targeted education. Now that hospitals can report and analyze data through the AU Option, the CDC’s focus on hospitals has shifted from encouraging AU reporting to using AU data to inform their stewardship efforts.
The CDC collaborated with hospitals that report data to the AU Option to provide a new resource in 2019: AU Option Case Examples. These case examples document success stories from hospitals that used their AU Option data for action to improve provider practices.
In 2014, the CDC called on all hospitals in the United States to implement antibiotic stewardship programs and released the Core Elements of Hospital Antibiotic Stewardship Programs to help hospitals achieve this goal. During this year’s USAAW, the CDC will release an update to this document that incorporates new evidence and lessons learned from experience with the Core Elements.
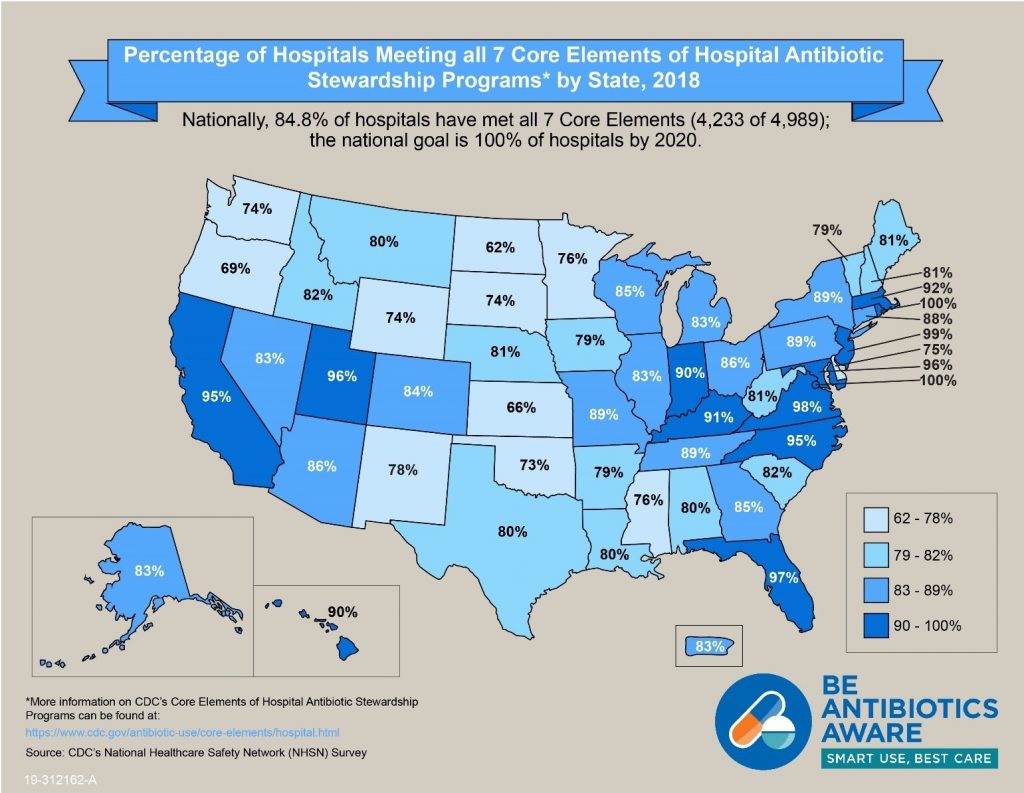
U.S. hospitals made great progress toward using AU data to combat antimicrobial resistance and improving patient outcomes through antimicrobial stewardship. As of 2018, 85% of acute care hospitals reported having all seven Core Elements in place, compared to only 41% in 2014.
The CDC provides resources to implement the Core Elements in a variety of healthcare settings—the NHSN AU Option helps fulfill both the tracking and reporting core elements. The more hospitals report to the NHSN AU Option, the more data CDC can leverage to develop benchmarks, recommendations, and best practices. These resources can help hospitals bridge the gap between AU data and action.
Do you have an NHSN AU Option success story to tell? Email NHSN@cdc.gov.

[1] Antibiotic Resistance Threats in the United States, 2019. Centers for Disease Control and Prevention. https://www.cdc.gov/drugresistance/biggest-threats.html
[2] Antimicrobial Stewardship. Association for Professionals in Infection Control and Epidemiology. https://apic.org/Professional-Practice/Practice-Resources/Antimicrobial-Stewardship/
[3] Davey P, Marwick CA, Scott CL, et al. Interventions to improve antibiotic prescribing practices for hospital inpatients. Cochrane Database Syst Rev 2017:2;CD003543.
[4] Ansari F, Gray K, Nathwani D, et al. Outcomes of an intervention to improve hospital antibiotic prescribing; interrupted time series with segmented regression analysis. J Antimicrob Chemother 2003;52:842-8.
[5] Solomon DH, Van Houten L, Glynn RJ. Academic detailing to improve use of broadspectrum antibiotics at an academic medical center. Arch Inter Med 2001;161:1897-902.